Diabetes mellitus – usually referred to simply as diabetes – is a chronic disease in which the body’s ability to produce or respond to the hormone insulin is impaired. This results in all sorts of health complications, not least the impact it can have on your feet.
What is diabetes?
Diabetes (the full terms is diabetes mellitus) is a type of endocrine disease. It is a metabolic disorder in which the body has high blood sugar levels for prolonged periods of time.
What are the different types of diabetes?
Diabetes type 1
Type 1 Diabetes is a result of an auto-immune destruction of pancreatic insulin producing cells.
Genetics, and pancreatic diseases can play a role in causing type 1 diabetes.
It is most common in young children, and is a lifelong condition to be managed.
Treatment includes lifestyle modifications and taking insulin to keep blood sugar levels under control.
Diabetes type 2
This condition results from insufficient production of insulin, causing high blood sugar.
Type 2 diabetes can occur when the body becomes resistant to insulin. Cells are not able to absorb glucose and convert it into energy as a result of this resistance.
Risk factors include age, as well as lifestyle choices such as smoking, lack of exercise, and obesity.
Genetics also plays a part in whether you develop type 2 diabetes.
Gestational diabetes
Gestational diabetes is a condition in which women develop diabetes (high blood sugar) during pregnancy. Initially, it may not cause any symptoms. Excessive thirst, sweating and frequent urination may be noticed as it progresses.
Urgent medical attention will be required to manage the condition.
What are the symptoms of diabetes?
Symptoms can include frequent urination, weight gain or loss, and excessive thirst or hunger. Slow healing of wounds, fatigue, and blurred vision can also occur. The complications resulting from diabetes are one of the main risks.
What effect can diabetes have on your feet?
Diabetes complications can have a serious effect on your feet. Having glucose levels that are too high in your blood can cause some significant foot problems.
There are two main foot problems associated with diabetes:
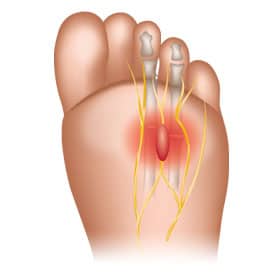
Diabetic neuropathy. This is where your diabetes causes nerve damage, and you may no longer retain the feeling in your legs and feet. The potential danger is that you therefore might not be aware of foot pain, which can lead to injuries going untreated, and cuts and sores becoming infected, which can cause a spiral of ever more serious health problems.
Nerve damage in the feet can also mean that you cannot control the muscles in that area properly, leading to mobility problems.
Peripheral vascular disease. Blood flow is also affected by diabetes. Poor blood flow means it will take longer for any foot injuries to heal, leaving you at greater risk of developing further conditions such as gangrene in your open wounds. Poor blood flow in the arms and legs is called peripheral vascular disease.
How do common foot conditions affect someone with diabetes?
As well as conditions specific to diabetes, sufferers will also have to contend with the increased risk that diabetes complications can create with common foot problems. While anyone can get one of the following conditions, if you are managing diabetes you face much more serious complications, such as the higher risk of infection and even amputation.
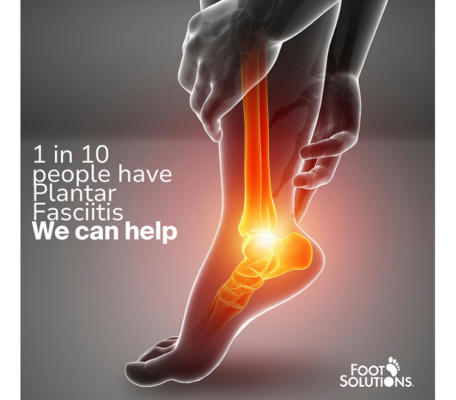
Plantar fasciitis
Plantar fasciitis is a condition resulting from the overstretching of the plantar fascia ligament, an overuse injury. Plantar fasciitis leads to heel pain and discomfort that can develop slowly throughout the day. A diabetic might find that losing weight can relieve pressure and help manage this condition.
Heel spurs
This is a bony protrusion from the heel bone, often associated with plantar fasciitis. A heel spur should hopefully not cause too many problems, but if it starts to cause uneven weight distribution that can increase the risk of other injuries or falling, which can have serious implications for anyone with underlying health issues.
Athlete’s foot
Athlete’s foot is a fungal infection, often caused by bacteria thriving on sweaty feet in tight shoes. The risk with athlete’s foot is that germs can enter through skin cracks and cause infection.
Dry skin
Similarly to athlete’s foot, the danger is of damaged skin allowing infection to take hold. A rigorous foot care and hygiene routine should be followed to limit the risk of diabetes complications.
Ingrown toenails
An ingrown toenail happens when the edge of a nail grows into your skin. This causes pain, redness, swelling, inflammation, and can easily lead to dangerous infection if you suffer from diabetes. Ill fitting shoes, badly maintained toenails, or trauma to the area can all prompt ingrown toenails, which are most common in the big toe.
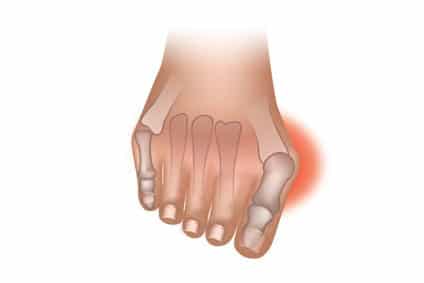
Hammer toe, claw foot
These are similar conditions that cause the shape of your foot to become deformed. The toe bends downward and the toe joint points to the sole of your shoe, causing mobility issues. Hammer or mallet toe can be a genetic condition, but it can also be caused by ill fitting shoes. Any of these conditions will likely lead to blisters, calluses and sores, and with them the risk of infection and further diabetes complications.
Plantar warts
These are caused by a virus and are usually painful. They often occur on the underside of the foot, meaning they are then compressed by walking and make physical activity uncomfortable. You may have to have them removed by a doctor.
Ulcers
These are deep breaks or sores in the skin. They can develop from minor cuts, scratches and abrasions to the skin, caused by shoes that rub or small accidents that do not seem at all serious. But if you have diabetes, and potentially slow healing wounds, ulcers can soon become established. It’s important to get them treated before they become infected.
Calluses and corns
These common foot problems have potentially greater implications for someone suffering from diabetes. Calluses and corns are similar conditions involving a build up of hard skin. They occur most commonly around the foot joints. While not presenting grave health concerns, they can easily lead to minor injuries and cracking that can become infected, and so they must be cared for appropriately.
How should someone with diabetes look after their foot health?
If you are managing diabetes, it’s still possible to maintain good foot health and minimize foot problems.
Take care of yourself. Follow your doctor’s advice, maintain a healthy diet, try and get your exercise in, and keep taking your medication. Monitor your blood sugar level and keep it at the recommended level.
Keep your feet really clean. Wash them every day in warm water. Take the temperature of the water before putting your feet in, in case you are suffering from diabetic neuropathy and might not feel a burn. Don’t soak your feet, but clean them thoroughly before completely drying them.
Check your feet daily for any cuts, sores or abrasions. Seek treatment if you have the slightest concern about a foot condition.
Use moisturizing lotion to care for the skin of your feet. Ask your doctor which lotion would be most appropriate.
Smooth corns and calluses after your bath or shower with an emery board. Go only in one direction and use only a gentle pressure to remove the dead skin.
Pay attention to your toenails. Clip them once a week, straight across. Don’t cut down the sides or at an angle as this increases the risk of ingrown toenails.
Always protect your feet by wearing shoes that enclose them, even around the house. Walking barefoot presents a huge risk.
Wear good quality proper shoes that fit well. Wearing poor fitting shoes is the cause of many foot problems that could have disastrous complications for a diabetic person.
Protect your feet. Check shoes don’t have objects left inside, and always make sure you are wearing shoes in more hazardous environments. Consider the temperature too – don’t let feet get too hot or too cold, and remember diabetic neuropathy may be affecting your ability to judge the temperature. Don’t wear high heels!
Encourage blood flow. Keep moving when you can, try and get some physical activity every day, and if nothing else wiggle your feet and flex your ankles to get blood into your extremities.
If you have a foot condition that requires treatment, get it straight away. Some that might seem simple, such as foot blisters, can turn into slow healing sores and become a big problem without the right medical help.
Check in regularly with a foot specialist, even if you don’t have any foot problems. It will set your mind at rest and you can’t be too careful.
Are you looking for ways to improve your foot health?
Whether you have diabetes or ingrown toenails, at Foot Solutions we can help. As experts in all things foot care, our range of specialist footwear caters for every foot need. From foot pads to physical therapy, we know how to relieve pain and help you step out in style and comfort. Perhaps you have diabetes and are thinking about better protection for your feet; or you are concerned that your tight calf muscles are caused by ill fitting shoes. Whatever your worry, come to Foot Solutions today, where our friendly team can help you put your best foot forward!